granulomatosis with polyangiitis
 Generated by DeepSeek V3.2
Generated by DeepSeek V3.2Expansion Funnel Raw 85 → Dedup 0 → NER 0 → Enqueued 0
| granulomatosis with polyangiitis | |
|---|---|
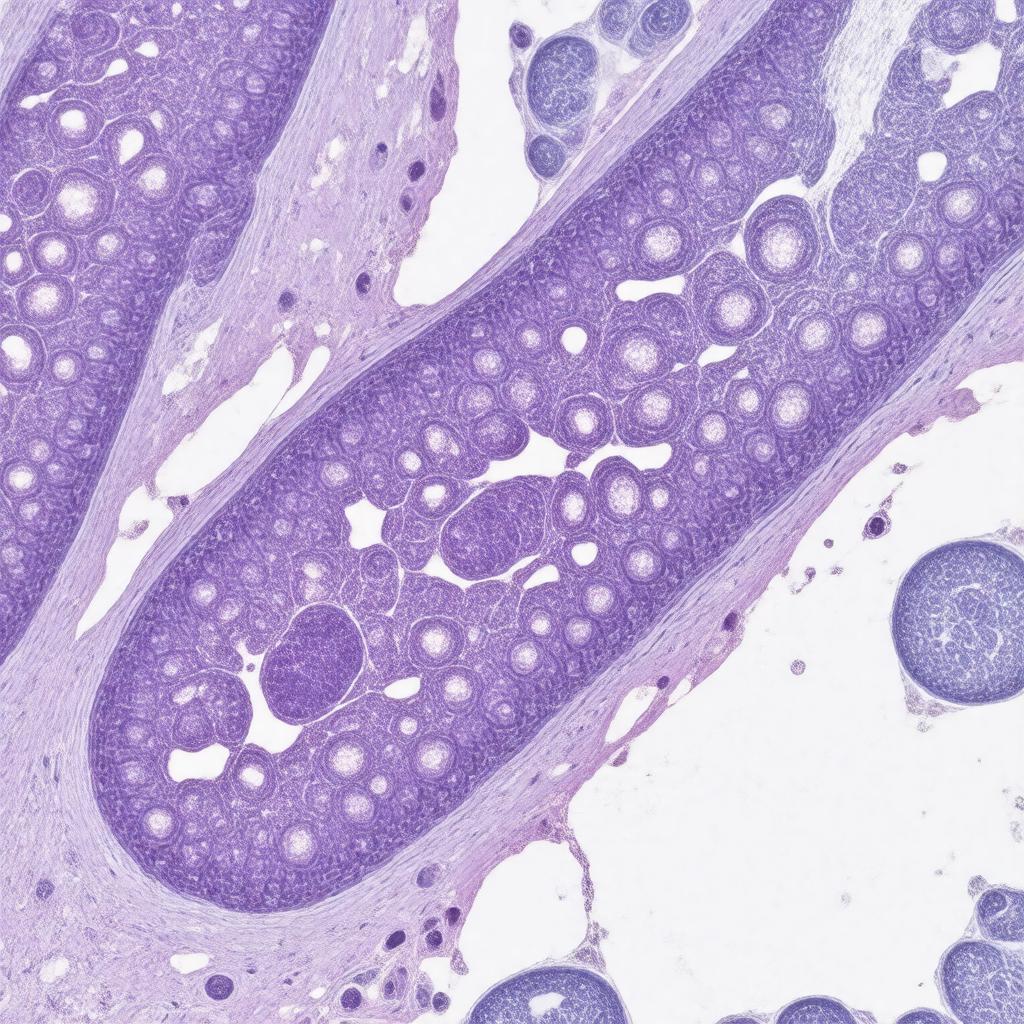 | |
| Name | Granulomatosis with polyangiitis |
| Synonyms | Wegener's granulomatosis |
| Field | Rheumatology, Nephrology, Pulmonology |
| Symptoms | Rhinitis, sinusitis, cough, hemoptysis, glomerulonephritis |
| Complications | Kidney failure, lung hemorrhage, subglottic stenosis |
| Onset | Any age, peak 40–65 |
| Duration | Chronic |
| Causes | Unknown |
| Diagnosis | ANCA testing, biopsy |
| Differential | Eosinophilic granulomatosis with polyangiitis, microscopic polyangiitis, Goodpasture syndrome |
| Treatment | Glucocorticoids, cyclophosphamide, rituximab |
| Prognosis | Relapsing-remitting |
| Frequency | 3–14 per million |
granulomatosis with polyangiitis is a rare, systemic form of vasculitis characterized by inflammation of blood vessels and the formation of granulomas. It primarily affects the respiratory tract and kidneys, leading to a wide array of potentially severe symptoms. The disease is strongly associated with antineutrophil cytoplasmic antibodies (ANCA), particularly those targeting proteinase 3. Management involves immunosuppressive therapy to induce and maintain remission.
Signs and symptoms
Initial manifestations often involve the upper respiratory tract, including persistent rhinitis, sinusitis, otitis media, and potentially destructive nasal septum perforation. Pulmonary involvement may present with cough, hemoptysis, pleuritic pain, and nodules visible on chest radiograph. Renal disease, typically a pauci-immune glomerulonephritis, can progress rapidly to kidney failure. Other common features include ocular inflammation such as scleritis or orbital pseudotumor, skin lesions like purpura or ulcers, and neuropathy, particularly mononeuritis multiplex. Constitutional symptoms like fever, fatigue, and weight loss are frequent.
Causes and pathophysiology
The exact cause remains unknown, but it is considered an autoimmune disease with a complex interplay of genetic and environmental factors. A key feature is the presence of ANCA, primarily of the cytoplasmic pattern (c-ANCA) targeting proteinase 3 within neutrophils. These antibodies are thought to activate primed neutrophils, leading to their adherence to endothelial cells and release of reactive oxygen species and proteolytic enzymes, causing vascular damage. The characteristic necrotizing granuloma formation, particularly in the respiratory tract, involves a cell-mediated immune response with T lymphocytes and macrophages. Some studies suggest potential triggers like chronic Staphylococcus aureus infection or exposure to silica.
Diagnosis
Diagnosis relies on a combination of clinical findings, serology, and histopathological evidence. Serological testing for ANCA, especially c-ANCA with specificity for proteinase 3, has high specificity but is not definitive alone. Tissue biopsy from an affected organ, such as the kidney, lung, or sinus mucosa, is often required for confirmation. Typical biopsy findings show necrotizing vasculitis of small to medium vessels, extracapillary glomerulonephritis (crescents) in the kidney, and geographic necrosis with granulomatous inflammation. Imaging studies like computed tomography of the sinuses or chest can identify characteristic lesions. Differential diagnoses include eosinophilic granulomatosis with polyangiitis, microscopic polyangiitis, and Goodpasture syndrome.
Treatment
Treatment is divided into induction of remission and maintenance therapy. For severe, organ-threatening disease, induction typically involves high-dose glucocorticoids combined with either cyclophosphamide or the anti-CD20 monoclonal antibody rituximab. The RAVE trial demonstrated the non-inferiority of rituximab to cyclophosphamide for induction. For maintenance of remission, agents like azathioprine, methotrexate, or continued rituximab are used, guided by trials such as the MAINRITSAN trial. Plasmapheresis may be added for severe renal involvement or diffuse alveolar hemorrhage. Prophylaxis against Pneumocystis jirovecii pneumonia with trimethoprim/sulfamethoxazole is standard.
Prognosis
Prior to the advent of effective immunosuppressive therapy with cyclophosphamide and glucocorticoids, the disease was often fatal within months. With modern treatment, remission is achieved in over 80% of patients, though relapses are common, occurring in approximately 50% within five years. Long-term prognosis is heavily influenced by the extent of renal damage at diagnosis and the occurrence of treatment-related complications, including infections from immunosuppression and malignancies related to cyclophosphamide exposure. Morbidity often results from chronic damage to organs like the kidneys, lungs, and sinuses.
Epidemiology
Granulomatosis with polyangiitis is a rare disease with an estimated annual incidence of 3 to 14 cases per million population in studies from Europe and North America. It can occur at any age but most commonly presents between the ages of 40 and 65. There is no strong gender predilection, with some studies showing a slight male predominance. The disease is more prevalent among individuals of Northern European descent. Seasonal variation and geographic clustering have been reported, supporting potential environmental influences, though no definitive causative agent has been identified.
Category:Autoimmune diseases Category:Vasculitides Category:Rheumatology